How effective is CPAP?
Real help or eternal crutch therapy
Real help or eternal crutch therapy
CPAP ventilation, BIPAP and ASV are forms of device-related overpressure breathing, which are regarded as gold standards in the therapy of obstructive sleep apnea syndrome. Devices for overpressure breathing quickly captured the cost-hit list of medical supplies and the trend is unbroken.But:
Because these are purely symptomatic treatments, patients have to use their “crutches” daily until to the grave, if they want to reduce their nighttime breathing problems. Regular checks of their sleep, hygiene and technology go nessecarily hand in hand. No wonder many users give up at any time: After all, the causes do not change, and every night without “crutches” makes this aware again.
This article was written in response to an article by the german medical newspaper “Ärzte Zeitung”:
Schlafapnoe: Schützt Beatmung doch vor Herzinfarkt?
New scientific findings relativize the promises of CPAP therapy - Read more
Scientific evidence for the various positive primary effects, the preventive effects against life-threatening diseases of the heart and brain are mainly derived from poorly potent studies, seemingly plausible explanations, manufacturer-financed documentation, as well as acclamations from experts and users. The implicit core statements of study results fulfill the criteria of a linear logic: If you breathe too little at night and do not supply your organs with sufficient oxygen, you must be close to the end!
Woe to him who rebukes!
Based on a clientele of several thousand patients and carried out with international participation, the recent studies relativize the previous assumptions. Investigations were conducted on 2717 patients from 89 centers in seven countries. In all, there was a sleep apnea syndrome and at the same time coronary heart disease, stroke or other cerebrovascular disease. It was found that the incidence of heart attacks, cerebral infarctions, heart failure, and deaths in those groups, which applied the pressure breathing apparatus, was not reduced but even increased.
By using a device for adaptive servo evacuation, which is mainly used in patients with Cheyne-Stokes breathing and is considered as a technical optimization of the PAP devices, the death rate increased significantly, even though the device drastically reduced the number of respiratory traps. Ulysses Magalang from the Wexner Medical Center, Columbus and Allan Pack from the Perelman School of Medicine in Philadelphia, among others, consider the components of the ventilation, i.a. the continuous positive airway pressure that the device generates as a possible cause. Also, the authors of the Jama study (2017), which is based on 7266 patients, could not detect a reduction in risk and death occurence in cardiovascular diseases, regardless of whether patients were provided with PAP devices or not.
Medical applications must primarily focus on the treatments of causes. Only in this way does the patient have the prospect of a healthy, independent life.
Continuous long-term symptomatic supply with devices (crutches) should not become the standard. Often their use has a spontaneous positive effect on the symptom. Negative changes that come along with it are usually introduced later and are not assigned to the primordial application. Long-term applications of “crutches” are never without consequences. At the very least, they cause compensatory changes of movement and function patterns. Neurophysiological changes affect the parasympathetic nervous system and organ activities.
This and more are the consequences of long-term pressure breathing. However, the authors do not want to question their application in principle. If it is important to optimize night-time breathing spontaneously, PAP methods are recommended. Previously or in parallel, however, additional procedures should be taken which also address the cause of the existing breathing problem. Thus, a lifelong and possibly negative device dependency may be avoided. In obstructive sleep apnea, tissue and muscles in the mouth and throat are relaxed. They constrict and obstruct the airways. Therefore, it is obvious to correct these underlying problems. As a rule, this can not be done surgically, but only by training of muscles and developing physiological patterns of movement and functions.
Whoever lends us crutches does not help us,
but who teaches us to walk. (Charles Tschopp)
In the treatment of the “No. 1 widespread disease” – back pain, the importance of muscles and function has long been recognised. In the past, spinal problems were usually treated by supporting and immobilising the spine in order to reduce supposedly harmful movements. Later operations of different techniques followed. In recent years, however, the far more successful training methods against back problems have become the “standard of art”. Those affected are mobilised. Muscles and posture are trained to stabilise the back.
For problems in the mouth, throat and breathing the treatment is still reduced to the approaches:
Crutches, supports and cutting.
In most cases, training is not on the agenda, although the mouth, throat, face, and head have as many muscles and the finest muscle chain functions as there is nowhere else in the human body. If functional and muscular deviations disrupt this fine-tuned system, a neurophysiological training is required for correction.
The evil at the root only can be combated in this way. The causes of narrowed or obstructed airways are to be treated with corrective exercises. As with the example of the back, consistent training is required.
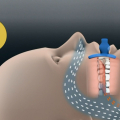
In the case of obstructive sleep apnea, relaxed tissue in the pharynx causes a recurring occlusion of the airways
For example, with FACEFORMER Therapy, an easy-to-perform but complex exercise program is available to the practitioner and the patient. It aims at treating the causes of snoring and sleep apnea. Slackened muscles are trained, incorrect movement patterns and malfunctions are corrected.
You can purchase your FaceFormer online in the Dr. Berndsen Shop, from our sales partners or from numerous doctors and therapists or locally in your pharmacy.
Ask for the central pharmaceutical number PZN 18092273 (FaceFormer ONE blue).
Further product variants and useful accessories are available.
Saving tip especially for doctors and therapists: 20%++ discount on orders of 5 FaceFormers or more!
The effective solution for snoring, sleep apnea, CMD, jaw problems and many other indications. Simple, causal, effective.
Der FaceFormer ONE Der FaceFormer, ein Medizinprodukt der Klasse 1, ist aus medizinischem Elastosil gefertigt und garantiert schadstofffrei. Die Therapie zielt darauf ab, fehlerhafte Funktionsabläufe zu korrigieren, die verschiedene Symptome beeinflussen können. Seit zwei Jahrzehnten stellt die FaceFormer-Therapie eine…
Die FaceFormer® Therapie: Der FaceFormer, ein Medizinprodukt der Klasse 1, ist aus medizinischem Elastosil gefertigt und garantiert schadstofffrei. Die Therapie zielt darauf ab, fehlerhafte Funktionsabläufe zu korrigieren, die verschiedene Symptome beeinflussen können. Seit zwei Jahrzehnten stellt die FaceFormer-Therap…
Der neue FaceFormer® ZERO Auf vielfachen Anwenderwunsch hat die FaceFormer Familie Zuwachs bekommen. Zusätzlich zum bekannten FaceFormer ONE in blau oder kristallklar ist ab sofort der FaceFormer ZERO erhältlich. Was ist anders? Der FaceFormer ZERO weist eine geringere Materialhärte auf, als die bisherigen Modelle. Grö…
FaceFormer® ZERO & ONE Therapie-Set für Erwachsene Überblick: Dieses Therapie-Set umfasst die Modelle FaceFormer ZERO und FaceFormer ONE. Beide sind als medizinische Geräte der Klasse 1 aus medizinischem Elastosil® hergestellt und sind BPA-frei sowie frei von flüchtigen Stoffen. Sie sind speziell darauf ausgelegt, die …
Wasserstr.25
59423 Unna
Germany
+49 (0) 23 03-89 99 1
+49 (0) 23 03 – 89 88 6
Mo. to Fr. from 8:00 to 16:00

 Treating snoring and sleep apnea – What you should know about
Treating snoring and sleep apnea – What you should know aboutThis site uses cookies. By continuing to browse the site, you are agreeing to our use of cookies.
OK, agree with allAgree to essentialsShow settingsThe satisfaction of visitors to our website is important to us. In order to better address you, we use cookies. Thereby we achieve that the website works technically reliable and secure.
You can change or revoke your consent at any time.
In the privacy policy you can learn more about cookies and privacy setting.
View privacy policy
Essential cookies enable basic functionality and are necessary for the proper functioning of the website.
This data may be linked to user information of users logged in on youtube.com and google.com.
YouTube video embedding
Used to unlock YouTube content.
Google Analytics
Cookie from Google for website analytics.
Generates statistical data about how the visitor uses the website
